Posterior Rami Blocks & RFTC
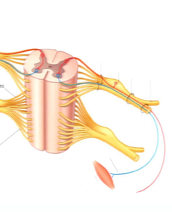
The posterior ramus of spinal nerve (or posterior primary division) refers to the posterior division of a spinal nerve. The ramus is also known by a number of other names, “posterior (or dorsal) rami (or branches or divisions) of the spinal nerves”. The posterior ramus is one of two major branches of a spinal nerve that emerge after the nerve emerges from the intervertebral foramen. The posterior ramus carries information that supplies muscles and sensation to the human back.
Structure:
Shortly after a spinal nerve exits the intervertebral foramen, it branches into the posterior ramus, anterior ramus, and rami communicantes. Each of these carries both sensory and motor information. After it is formed, the posterior ramus (plural: rami) of each spinal nerve is travels backward, except for the first cervical, the fourth and fifth sacral, and the coccygeal.
Posterior rami divide into medial and lateral branches which supply muscles and skin of the back. The medial branch (Latin: rami medialis) also supplies articular branches to the zygopophyseal joints and the periosteum of the vertebral arch. In the neck and upper back, the medial branch continues through the deep and superficial back muscles to supply overlying skin; in the lower back, the lateral branch does this.
Nomina Anatomica lists dorsal primary rami as “rami dorsales” for each group of spinal nerves:
- Cervical (nervorum cervicalium)
- Thoracic (nervorum thoracicorum)
- Lumbar (nervorum lumbalium)
- Sacral (nervorum sacralium)
- coccygeal (nervi coccygei)
Function
Because each spinal nerve carries both sensory and motor information, spinal nerves are referred to as “mixed nerves.” Posterior rami carry visceral motor, somatic motor, and sensory information to and from the skin and deep muscles of the back. The posterior rami remain distinct from each other, and each innervates a narrow strip of skin and muscle along the back, more or less at the level from which the ramus leaves the spinal nerve.
RADIO FREQUENCY PROCEDURES
Radio Frequency (RF) Nerve Ablation (also known as RF Rhizotomy) is a therapeutic procedure designed to decrease or eliminate pain symptoms within spinal facets by temporarily deactivating minor nerves around the spine. The pain generating nerves for many patients are often small, unimportant fibers which can cause severe pain. These nerves can be temporarily shut down using radiofrequency energy to heat the surrounding tissue and deactivate the pain generating nerve fibers.
The procedure is performed by accessing the affected nerve under x-ray guidance. Once properly positioned, a special probe is advanced allowing the delivery of radiofrequency energy to the targeted area. An electric current is then used to cauterize the sensory nerves that innervate the facet joint(s).
Before patients can be scheduled for an RF rhizotomy procedure, they generally must undergo a series of facet injections to verify the exact source of their symptoms. These tests may require several visits. If a patient’s pain can be taken away or significantly relieved with a local anesthetic block for a short term, then blocking the nerves with Radiofrequency denervation will usually give long term or even permanent relief. If successful, the pain relief following an RF procedure can last considerably longer than relief following local anesthetic and steroid blocks (Results can last from months to years.)
This process can be used on any area of the spine, cervical, thoracic, or lumbar. Due to the trauma to the nerve, you may experience an increase in symptoms for 5-7 days after the procedure. Pain relief benefits should be apparent within 2-4 weeks.

